Hassle-Free Prior Authorizations So You Can Focus on Care
At MindBridge RCM, we understand the critical role prior authorization plays in ensuring timely access to essential healthcare services. Our comprehensive prior authorization solutions streamline the process, reduce administrative burden, and accelerate approvals—allowing healthcare providers to focus on delivering exceptional patient care.

Streamlined Credentialing for Faster Insurance Approval
At MindBridge RCM, we provide comprehensive credentialing services that verify healthcare providers’ qualifications, manage documentation, and secure agreements with insurance companies. By ensuring full compliance with industry standards, we help providers gain insurance approval efficiently, minimizing delays and administrative burdens. Partner with us for a seamless process that keeps your practice running smoothly and fully compliant.
Grow with Ease
Scale your healthcare practice smoothly and adapt to new payment models at your own pace—without adding staff. Our streamlined revenue cycle processes support sustainable growth while minimizing complexity and overhead, so you can stay focused on long-term success.
Speed Up Getting Paid
Top healthcare providers trust AR Rescue’s RCM services to process claims accurately and efficiently, ensuring faster payments and improved cash flow.
Get your time back
Eliminate the need for additional staff or the time and resources spent training billers. Focus on patient care while we efficiently manage your billing for you.

Numbers That Tell Our Story
” BEHIND EVERY STAT IS A MILESTONE WE ARE PROUD OF “
YEARS IN BUSINESS
CLAIMED PROCESSED
REVENUE IMPROVEMENT
REVENUE IMPROVEMENT
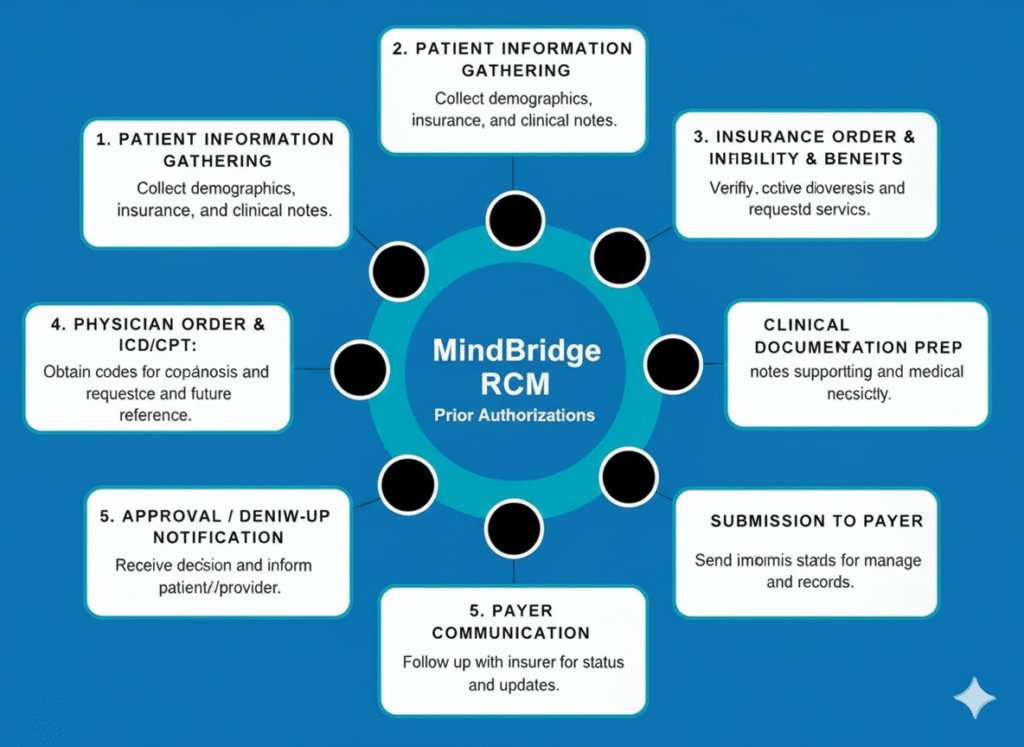
Prior Authorization Support That Speeds Approvals, Reduces Delays, and Safeguards Your Revenue
Eliminate Insurance Delays with Proactive Prior Authorization Management
Prior authorization is one of the most time-critical and detail-driven processes in healthcare, where even minor errors or delays can interrupt patient care and impact reimbursements. Evocare Billings handles the entire authorization process from beginning to end—verifying benefits, preparing precise documentation, and maintaining ongoing follow-ups with payers to secure quicker approvals and reduce denials. Our experienced billing specialists closely track every authorization, identifying and resolving potential issues before they cause delays. The result is smoother workflows, uninterrupted patient care, and a healthier, more predictable revenue stream for your practice.


Lift the Administrative Load and Restore Focus on Patient Care
Prior authorization responsibilities can overwhelm clinical and administrative teams, diverting valuable time away from patients and reducing operational efficiency. Evocare Billings removes this burden through streamlined workflows and deep payer-specific expertise that accelerate turnaround times while ensuring full compliance. Our dedicated authorization specialists manage the complexities end to end, allowing your staff to stay focused on what matters most—patient care. By simplifying authorization processes, we help improve productivity, reduce staff burnout, and create a more efficient, stress-free practice environment.

