Comprehensive Insurance Eligibility Verification for Your Medical Practice
Our experienced insurance verification specialists streamline medical coverage verification across the USA, ensuring accurate benefits confirmation, fewer claim denials, and a smoother experience for both providers and patients.

Why Eligibility Verification Services Are Essential for Accurate Medical Insurance Billing
Eligibility Verification Services (EVS) confirm whether individuals qualify for specific programs or benefits by accurately reviewing and validating coverage details. Our medical insurance verification specialists thoroughly analyze patient and policy information to ensure eligibility is confirmed upfront—helping streamline approvals, prevent coverage issues, and ensure the right services are provided to the right patients with confidence and efficiency.
Grow with Ease
Scale your healthcare practice smoothly and adapt to new payment models at your own pace—without adding staff. Our streamlined revenue cycle processes support sustainable growth while minimizing complexity and overhead, so you can stay focused on long-term success.
Speed Up Getting Paid
Top healthcare providers trust AR Rescue’s RCM services to process claims accurately and efficiently, ensuring faster payments and improved cash flow.
Get your time back
Eliminate the need for additional staff or the time and resources spent training billers. Focus on patient care while we efficiently manage your billing for you.

Numbers That Tell Our Story
” BEHIND EVERY STAT IS A MILESTONE WE ARE PROUD OF “
YEARS IN BUSINESS
CLAIMED PROCESSED
REVENUE IMPROVEMENT
REVENUE IMPROVEMENT
MindBridge RCM’s Health Insurance Eligibility Verification Services
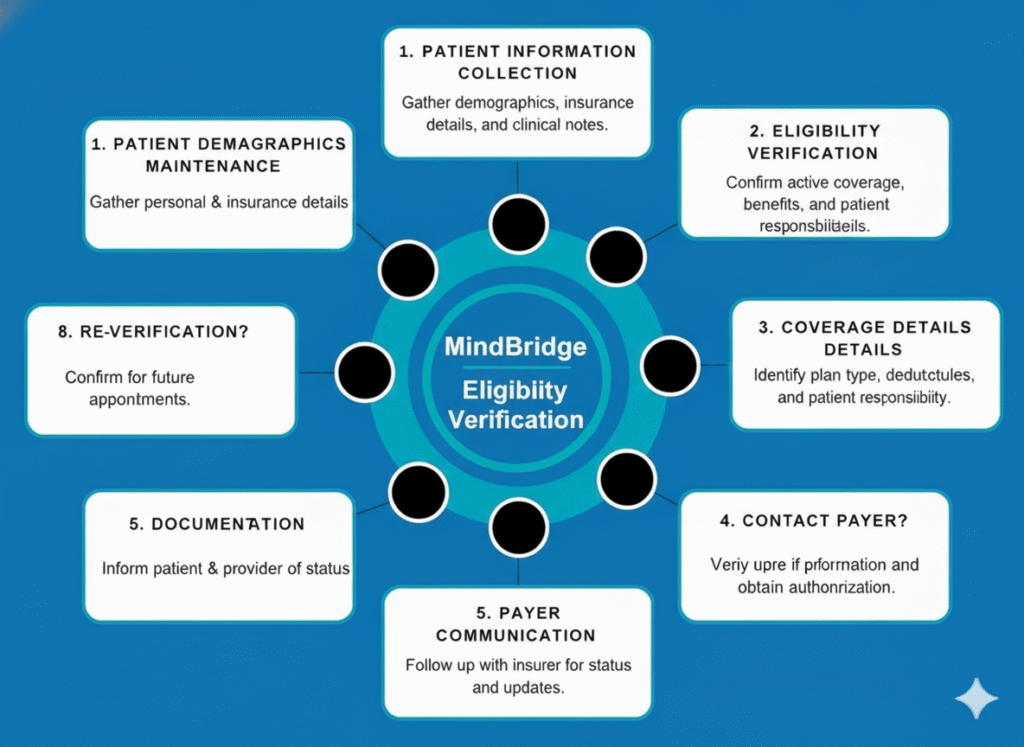
Our Patient Eligibility Verification Approach
Discover how MindBridge RCM simplifies and streamlines insurance eligibility verification with a precise, efficient, and reliable process that ensures accurate coverage confirmation, faster workflows, and a smoother experience for both providers and patients.


MindBridge RCM’s End-to-End Eligibility Verification Workflow
- Seamless Schedule Integration: Securely receive patient schedules from hospitals and clinics via encrypted email or FTP, ensuring timely and accurate updates.
- Comprehensive Insurance Coverage Verification: Verify patient coverage with all primary and secondary payers to confirm benefits and prevent billing errors.
- Accurate Demographic Validation: Review and validate patient demographic information to ensure completeness and accuracy from the start.
- Proactive Account Maintenance: Keep patient accounts current by updating all insurance and personal details in real time.
- Clear Patient Communication: Collaborate directly with patients to quickly obtain any additional information needed to complete the verification process.
- Precise Billing System Updates: Enter critical data—member and group IDs, coverage effective dates, termination dates, and co-pay details—into the billing system to support accurate claims submission and timely reimbursement.
Billing With Us !
Streamline Your Workflow & Boot Productivity With Our Innovative Solutions