Efficient Claim Rejection and Denial Management with MindBridge RCM
At MindBridge RCM, we specialize in identifying, analyzing, and resolving claim rejections and denials to protect your revenue and optimize cash flow. Our expert team investigates every denied or rejected claim, determines the root cause, and takes corrective action to ensure resubmission success. By streamlining the denial management process, MindBridge RCM helps reduce recurring errors, accelerate reimbursements, and maintain a healthy revenue cycle, giving your practice the financial stability and efficiency it deserves.

Comprehensive Rejection and Denial Management Services with MindBridge RCM
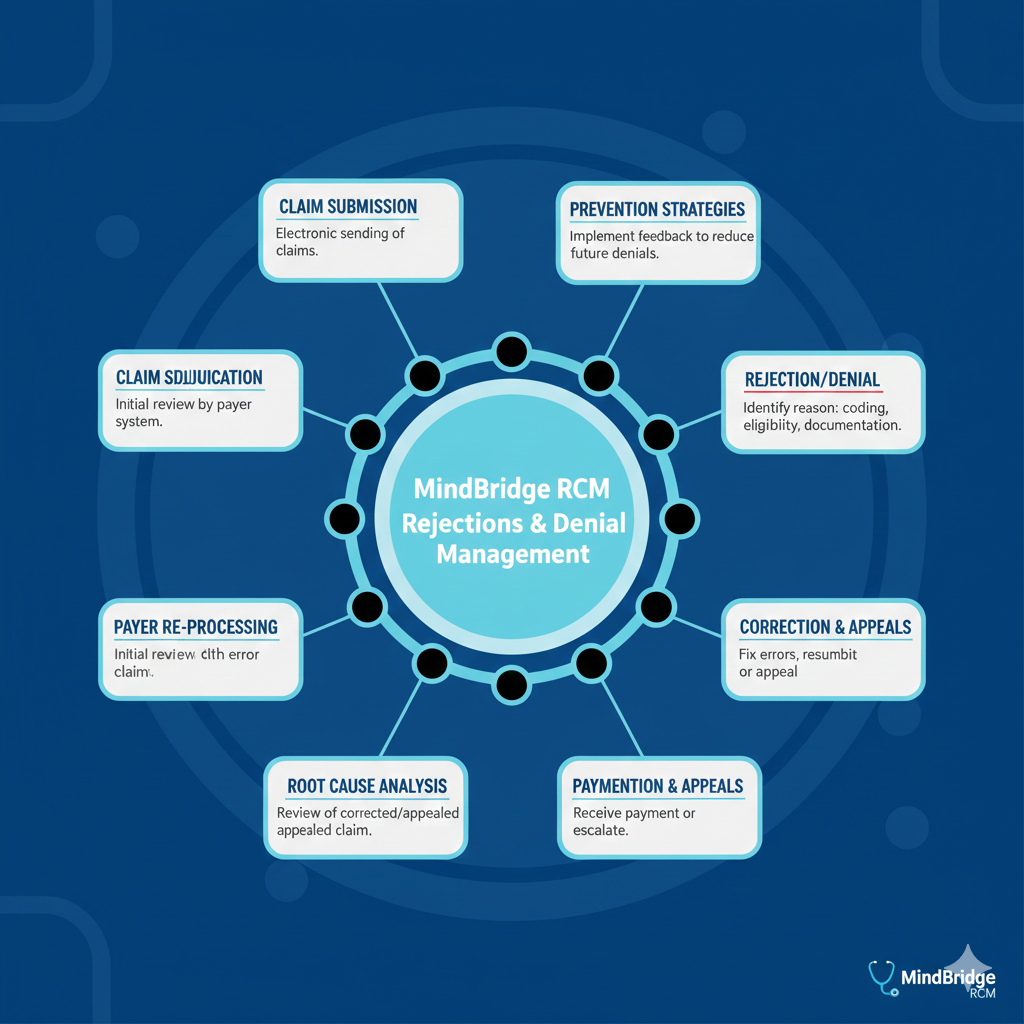
At MindBridge RCM, our denial management services improve medical billing efficiency by quickly identifying, analyzing, and resolving claim denials. By reducing rework, minimizing revenue loss, and accelerating reimbursements, we optimize your practice’s cash flow and overall operations. Our proactive approach—including root cause analysis and systematic tracking—ensures greater claim accuracy, compliance with payer regulations, and a smoother, more reliable revenue cycle.
Grow with Ease
Scale your healthcare practice smoothly and adapt to new payment models at your own pace—without adding staff. Our streamlined revenue cycle processes support sustainable growth while minimizing complexity and overhead, so you can stay focused on long-term success.
Speed Up Getting Paid
Top healthcare providers trust AR Rescue’s RCM services to process claims accurately and efficiently, ensuring faster payments and improved cash flow.
Get your time back
Eliminate the need for additional staff or the time and resources spent training billers. Focus on patient care while we efficiently manage your billing for you.

Numbers That Tell Our Story
” BEHIND EVERY STAT IS A MILESTONE WE ARE PROUD OF “
YEARS IN BUSINESS
CLAIMED PROCESSED
REVENUE IMPROVEMENT
REVENUE IMPROVEMENT
How MindBridge RCM’s Denial Management Boosts Medical Billing Efficiency
Why MindBridge RCM’s Denial Management Is Essential for Medical Billing
Denial management is a critical service that healthcare providers cannot overlook, as unresolved denials can delay reimbursements and negatively impact revenue. At MindBridge RCM, we handle claim denials efficiently to improve cash flow, reduce administrative headaches, and enhance patient satisfaction. Our best practices include categorizing denials, thorough claim scrubbing, monitoring performance, and managing the appeals process—ensuring faster resolutions, optimized revenue, and a smoother billing workflow for your practice.


Minimize Denied Claims and Accelerate Reimbursements with MindBridge RCM
At MindBridge RCM, our denial management services are designed to reduce claim denials and ensure timely reimbursements for your practice. Our expert team investigates every denied claim, identifies root causes, corrects internal errors, and implements permanent solutions to prevent future reoccurrences. By submitting accurate, mistake-free claims, we help practices achieve faster payments, optimize cash flow, and experience significant improvements in revenue recovery.

